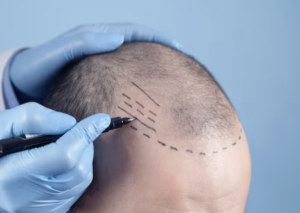
Hair Transplantation in Scalp Psoriasis and Other Skin Conditions
Chronic inflammatory skin conditions—such as scalp psoriasis, seborrheic dermatitis, lichen planopilaris, eczema, atopic dermatitis, or primary scarring alopecia—can pose additional challenges for hair transplantation. Patients often ask:
- Is hair transplantation possible with these conditions?
- How should I prepare?
- How long after remission can the procedure be done?
- Will transplanted hair survive, and which method is best—FUE, DHI, or manual?
Below are expert answers and evidence-based facts from medical literature.
How Inflammatory Skin Conditions Affect Hair Transplantation
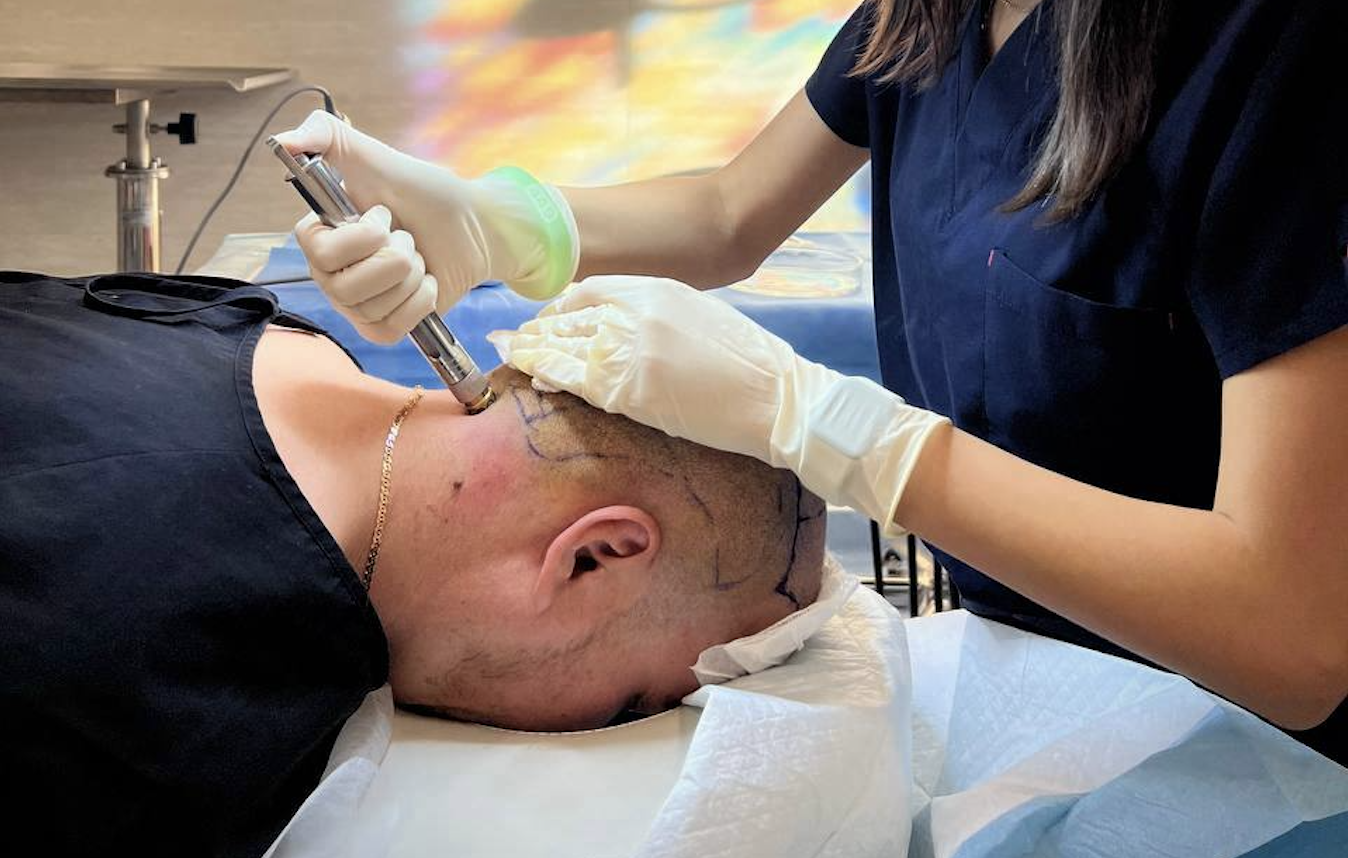
Inflammation in the scalp disrupts microcirculation, activates immune cells, and can damage hair follicles. This may reduce the success of hair transplantation, especially during active disease. For example:
- Psoriasis causes redness, scaling, and inflammation, creating an unfavorable environment for graft survival.
- Seborrheic dermatitis and eczema bring irritation, itching, and a disrupted skin barrier, which may also reduce graft quality.
- Scarring alopecia involves structural skin damage with completely destroyed follicles, requiring special attention.
Key point: Active inflammation is a direct contraindication for transplantation until the disease is in stable remission.
Scientific Evidence on Hair Transplantation in Inflammatory Skin Conditions
While studies specifically on psoriasis are limited, broader research on hair transplantation in chronic inflammatory scalp conditions—including scarring alopecia—provides useful insights:
Graft Survival
A prospective international systematic review examined follicular unit survival in primary scarring alopecia, an inflammatory condition of the scalp similar to severe psoriasis:
- 82.7 % survival at 7–12 months post-transplant
- 73.3 % at 13–24 months
- 58.4 % at 25–36 months
- 55.4 % at 37–48 months
- 39.6 % at 49–72 months
This shows that initial graft survival can be high, but gradually decreases over time, particularly if chronic inflammation persists.
Other Studies
A review of 33 publications on hair transplantation in various forms of inflammatory alopecia (including lichen planopilaris and scarring forms) found:
- ~87.8 % of patients experienced positive hair growth post-transplant, ranging from moderate (~40 % survival) to high (>90 %).
- Outcomes were most stable in patients with well-controlled inflammation and when modern hair transplant techniques were used.
Hair Transplantation Specifically in Psoriasis
Data on hair transplantation for patients with scalp psoriasis is limited, but clinical case reports indicate:
- In a series of 7 patients with chronic plaque psoriasis, most tolerated hair transplantation without worsening their condition.
- One patient developed a pustular flare post-transplant as a reaction to skin trauma, which was successfully managed with medication without compromising the grafts.
- Dermatologists highlight the risk of Koebner phenomenon, where skin trauma (including surgical incisions) can trigger new psoriatic plaques. Active psoriasis must be fully controlled before surgery.
We invite you to watch a video featuring a real patient story who underwent a hair transplant in Turkey with psoriasis and sensitive scalp.
This video will be useful for those who:
— are dealing with psoriasis or chronic scalp issues
— are unsure whether hair transplantation in Turkey is possible in complex cases
— are looking for honest information without promises or exaggeration.
Timing: When Can Hair Transplantation Be Performed?
Hair transplantation should only be performed once scalp inflammation is in stable remission.
Clinical recommendations:
- For inflammatory conditions like psoriasis or dermatitis: at least 6–12 months of stable remission before hair transplantation is optimal.
- For scarring forms (e.g., lichen planopilaris): many experts recommend waiting 2–5 years of remission before the procedure to reduce the risk of inflammation recurrence in the grafted area.
Preparing for Hair Transplantation in Skin Conditions
Proper preparation is essential:
- Assessment and Control of Inflammation
- Consult both a dermatologist and a hair specialist (trichologist).
- Treat psoriasis with medicated shampoos, topical steroids, or immunomodulators until symptoms are fully controlled.
- Systemic therapy may be needed under medical supervision.
- Donor Area Assessment
- Skin conditions should not affect the donor site.
- Donor area must be healthy and free from inflammation.
- Laboratory and Diagnostic Tests
- Scalp biopsy to rule out active inflammation.
- Dermoscopy to evaluate skin and follicle health.
Choosing the Hair Transplant Method
Modern hair transplantation techniques vary in skin trauma, and the method should be individualized:
- FUE (Follicular Unit Extraction)
- Most common and minimally invasive.
- Transplants individual follicular units.
- Minimal scarring, flexible donor/recipient zones.
- Well-suited for sensitive skin.
- DHI (Direct Hair Implantation)
- Hair is implanted directly without creating incisions first.
- More precise graft placement, less time outside the body.
- Ideal for highly reactive skin.
- Manual / FUT (Strip Method) ❌
- Higher trauma, more scarring.
- Less preferred for inflammatory skin conditions.
Fill out the form now and receive a personalized hair transplant plan, individual recommendations, and a free consultation with our specialists!
After Transplant: Hair Growth and Prognosis
- Transplanted hairs usually shed in the first 2–4 weeks (normal telogen phase).
- New growth begins at 3–4 months, improving up to 12–18 months.
- With stable remission and proper care, grafts have a strong chance of long-term growth, comparable to patients without skin disease.
Post-Transplant Care for Psoriasis and Other Skin Conditions
Patients with chronic skin conditions require special care to promote healing, scalp health, and graft survival:
- Gentle Scalp Care
- Use mild shampoos designed for sensitive scalps.
- Medicated shampoos (e.g., Glasso) are suitable for daily or regular use after wound healing, reduce itching, control scaling, and do not irritate grafts.
- Avoid harsh shampoos, home remedies with essential oils, or chemical irritants.
- Dermatologist-Supervised Maintenance
- Continue psoriasis or dermatitis treatment.
- Use topical corticosteroids, immunomodulators, or soothing agents as recommended.
- Regular dermatology check-ups help prevent disease relapse, which is critical for long-term graft growth.
- PRP Therapy for Hair Growth
- PRP (Platelet-Rich Plasma) stimulates graft growth, improves microcirculation, and promotes healing.
- Should only be used during stable remission to avoid triggering inflammation.
- Suggested protocol: begin 1–2 months post-transplant, monthly for 3–4 months.
- General Recommendations
- Timely follow-ups with your hair transplant surgeon to assess graft survival.
- Protect the scalp from sunburn, trauma, and friction for 2–3 months post-op.
- Avoid chemical treatments, coloring, or heat styling until full scalp recovery and graft integration.
A combination of mild medicated shampoos (e.g., Glasso), dermatologist-guided maintenance, and PRP therapy post-transplant can improve graft survival, accelerate hair growth, and maintain scalp health. The key is performing procedures only during stable disease remission and under specialist supervision.
Key Takeaways for Patients
- Hair transplantation is possible for patients with psoriasis or other chronic skin conditions, but only when the scalp is in stable remission and inflammation is fully controlled.
- Active inflammation can reduce graft survival, but with stable remission, outcomes are often comparable to patients without skin disease.
- FUE and DHI methods yield the best results due to minimal trauma and reduced risk of skin damage.
- Success depends on careful preparation, inflammation control, and ongoing dermatologist involvement from pre-op planning through post-op care and graft maintenance.